Knee osteoarthritis is painful on its own, but one of its most serious consequences is an increased risk of falls and related injuries. People with knee OA are more likely to trip, lose their balance, or feel their legs suddenly “give way,” which can lead to fractures and loss of independence. Understanding why this happens is the first step in protecting yourself or your patients.
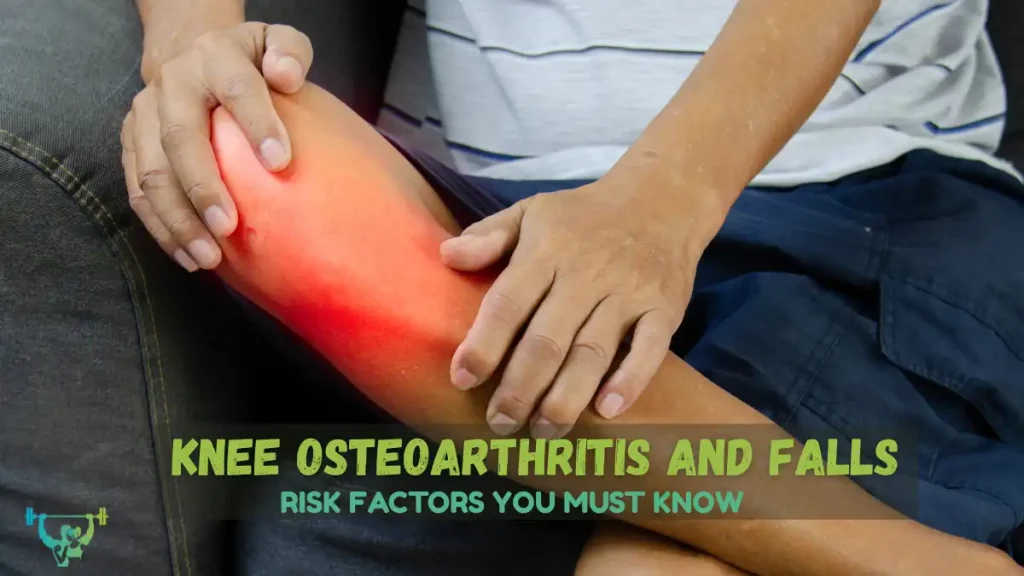
Falls are not just “accidents”; they are often predictable outcomes of specific physical and personal risk factors that can be identified and improved.
How Knee Osteoarthritis Increases Fall Risk
Knee osteoarthritis affects the joint surfaces, surrounding muscles, and how you move. Pain, stiffness, and swelling make it harder to control the knee and maintain a stable, efficient gait.
Common ways knee OA promotes falls include:
- Pain that makes you walk slower, limp, or avoid putting weight on one leg.
- Stiffness that reduces your knee’s ability to bend and adapt to uneven surfaces or obstacles.
- Muscle weakness that makes it hard to catch yourself if you stumble.
- Joint instability, where the knee feels like it might buckle or slide unexpectedly.
Over time, fear of falling may cause people to move less, which further weakens muscles and balance and actually increases fall risk.
Evidence-Based Risk Factors for Falls in Knee Osteoarthritis
A major systematic review on knee OA and falls found several consistent risk factors across 11 studies:
- Impaired balance: Difficulty maintaining steady posture when standing or walking.
- Muscle weakness: Especially in quadriceps and hip muscles, which are essential for standing and stepping.
- Multiple comorbidities: Conditions like diabetes, low back pain, or cardiovascular disease that compound functional limitations.
- More symptomatic joints: When both knees or the knee plus hip/ankle are painful, falls are more likely.
Knee pain itself was identified as a possible risk factor, but the strength of evidence was labeled “conflicting” because not all studies showed the same pattern. Limited evidence also pointed to knee instability, impaired proprioception (joint position sense), and the use of walking aids as potential contributors.
More recent cross‑sectional work has highlighted additional predictors of falls in knee OA:
- Higher symptom burden (higher KOOS symptom scores).
- Greater fear of falling.
- Reduced range of motion and poorer proprioception.
- Higher body mass index.
- Low back pain and diabetes.
Modifiable vs Non-Modifiable Risk Factors
Not every risk factor can be changed, but many can be improved.
Non‑modifiable factors:
- Age.
- Long‑standing structural joint damage.
- Past injuries or surgeries.
- Some chronic conditions that cannot be reversed.
Modifiable factors:
- Muscle strength and power.
- Balance and proprioception.
- Body weight and fitness level.
- Home environment hazards.
- Vitamin D levels, vision, and some medications.
Focusing on modifiable risk factors gives you a clear target for fall‑prevention strategies.
Simple Ways to Check Your Fall Risk at Home
These simple checks are not full clinical assessments, but they can give you an idea of how stable you are:
Chair stand test:
- Cross arms over chest and see how many times you can stand up and sit down from a standard chair in 30 seconds.
- Very low numbers or inability to perform may signal leg weakness.
Single‑leg stance (with support nearby):
- Stand near a counter or sturdy chair.
- Try balancing on one leg for up to 10 seconds, holding support if needed.
- Marked difficulty suggests balance deficits.
Timed up‑and‑go (TUG):
- Sit in a chair, then stand, walk 3 meters, turn, walk back, and sit.
- Longer times are associated with higher fall risk, especially in older adults.
Struggling with these tests is a strong signal to seek a professional assessment and begin targeted strength and balance training.
Fall Prevention Strategies for Adults With Knee Osteoarthritis
For adults with knee OA, fall prevention should be part of routine care.
1. Strength and balance training
- Quadriceps and hip strengthening (squats to chair, step‑ups, hip abduction).
- Balance drills: tandem stance, single‑leg stance, heel‑to‑toe walking.
- Consider supervised physiotherapy to ensure safe technique.
2. Home safety upgrades
- Improve lighting in hallways and bathrooms.
- Remove loose rugs and clutter.
- Install grab bars in bathrooms and railings on stairs.
- Use non‑slip mats and supportive footwear.
3. Managing comorbidities and medications
- Optimize diabetes control and blood pressure.
- Review sedative or blood pressure medications that may cause dizziness.
- Address low back pain and other sources of gait disturbance.
When to Seek Professional Help
Seek medical or physiotherapy help if you:
- Have had one or more falls in the past year.
- Feel your knee “gives way” regularly.
- Notice sudden worsening of pain, swelling, or instability.
- Develop new neurological signs like numbness or weakness in multiple limbs.
Specialists can identify your personal fall risk profile and build a tailored program to reduce it.
FAQs About Knee Osteoarthritis and Falls
Yes. People with knee osteoarthritis fall more often than similar adults without knee OA, mainly due to pain, muscle weakness, impaired balance, and multiple joint symptoms.
Those with poor balance, weak leg muscles, multiple painful joints, fear of falling, higher BMI, and comorbidities like diabetes or low back pain have higher fall rates.
Yes. Fear of falling is strongly associated with actual falls and reduced activity, which in turn weakens muscles and increases fall risk, creating a vicious cycle.
Targeted strengthening and balance training can improve proprioception, ROM, and confidence, all of which are protective against falls in people with knee osteoarthritis.

